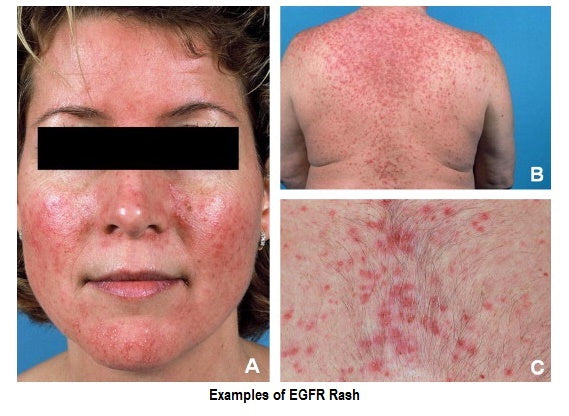
Chemo Rash (EGFR Rash)
What is EGFR Rash?
Chemo Rash, which is also known as EGFR Rash, is a common skin-related side effect of certain chemotherapy medications.
The dry skin rash is typically characterized by mild scaling, pimples, roughness, a feeling of tightness, and possibly itching and burning on the skin of the face. Also known as maculopapular rash- macular means small flat areas and papular means small raised lesions – the rash may range in color from light pink to bright red and the affected area may feel hot.
Chemo rash is usually preceded by redness of the skin or a warm sensation on the face that may feel like sunburn. Sometimes the rash leads to peeling and lesions as well. Acne-like red bumps, often forming in clusters commonly appear on the face, neck, chest, scalp, and back.
Many commonly-used chemotherapy medications can cause EGFR Rash, including Iressa (generic name: gefitinib), Tarceva (erlotinib), Erbitux (cetuximab), Tykerb (lapatinib), Vectibix (panitumumab), Caprelsa (vandetanib), and tyrosine kinase inhibitors.
Alternate & Related Terms: Maculopapular rash, acneform* rash, acneiform* rash, Tarceva Rash, Erbitux rash, chemo rash, HER1 rash, folliculitis
* - NOTE: Because EGFR rashes are in no way related to acne, and because traditional acne treatments can make symptoms worse, most dermatologists and oncologists now recommend against the use of the outdated & confusing term “acneiform” or “acneform”.
Common Symptoms of Chemo Rash
EGFR Rash develops in 50% to 75% of patients and usually occurs within the first few weeks of starting an EGFR antagonist. Skin reactions can be independent of dose and can persist long after drug therapy has been discontinued.
General symptoms may include the following:
- Pimples and red bumps on the face, neck and upper chest or back
- Tenderness of facial skin, with a sunburn-like sensation
- Itchiness, especially the scalp
- Tender sores inside the nose, corners of the mouth or eyes
- Inflammation around nails (paronychia), especially the thumbs
- Nails that become brittle and may loosen from the nail bed
- Hair loss over the entire scalp and decreased hair on legs or arms
- Increased growth and curling of the eyelashes and eyebrows
- Easily bruised skin
- Dry, flaky skin
- Dry, itchy eyes
If you do experience chemotherapy rash while undergoing treatment, this can be very good news despite the painful nature of the rash. The reason is because the rash. The skin side effects you may experience with an EGFR inhibitor are not a sign of an allergic reaction or infection.

EGFR Rash Skin Care and Management
First and foremost, follow your doctor’s instructions. Taking your medication at the right time of day and in the prescribed dosage is important to your well-being and your recovery. Your doctor may temporarily stop treatment if your skin rash is too uncomfortable for you. This is something you should discuss with your doctor and not take upon yourself.
EGFR rash seems to feel better with intense hydration. This helps relieve the redness, irritation, and dryness that’s affecting the skin. The affected area should never be treated with drying agents designed to fight acne. A hydrating moisturizer or lightweight serum is best for maintaining the skin.
Additional recommendations for effective Chemo Rash treatment:
- Use only mild, hypo-allergenic soap. Avoid antibacterial soaps, as they are more drying.
- Avoid hot baths. This will further dry your skin. Take a quick, warm shower instead.
- Pat yourself dry with a towel instead of rubbing your skin.
- Use a thick, quality moisturizer, avoiding alcohol, dyes, and fragrances.
- Avoid exposure to the sun. Always use a sunscreen with a sun protection factor (SPF) of at least 30. Choose a product for sensitive skin (e.g., one that contains zinc oxide or titanium dioxide). Reapply sunscreen after 2 hours of continuous exposure.
- Remove all makeup with gentle cleansers.
- Avoid perfume, cologne or aftershave that contains alcohol.
- Avoid wearing clothing such as wool next to your skin that will make your skin feel itchy.
Skincare and Regimens for Face Rash
Like most skin care regimens, a preventative regimen is usually the most effective for maintaining control over the skin, so cancer patients undergoing EGFR inhibitor treatment may want to begin with moisturizer and anti-oxidants as early as possible during treatment. Lindi Skin's serums, washes, and moisturizers have been clinically proven to help reduce skin toxicity and improve the quality of life of those who have used them.
NOTE: We strongly encourage you to talk with your health care professional about your specific medical condition and treatments. The information provided in this Web site about skin reactions and other medical conditions is meant to be helpful and educational, but is not a substitute for professional medical advice. Free samples limited to 1 per houshold.

